ABOUT THE DISEASE
The pancreas is a large gland in the abdomen located behind the stomach and next to the upper part of the small intestine and liver. The pancreas has two main functions:
1. Secreting powerful digestive enzymes into the small intestine to aid the digestion of carbohydrates, proteins, and fat.
2. Regulating blood glucose metabolism by releasing the hormones insulin and glucagon into the bloodstream.
Pancreatitis is a disease in which there is inflammation of the pancreas. In very severe cases, pancreatitis can result in bleeding into the gland, serious tissue damage, infection, and cyst formation. Severe pancreatitis can also damage other vital organs such as the heart, lungs, and kidneys if enzymes and toxins are released into the bloodstream.
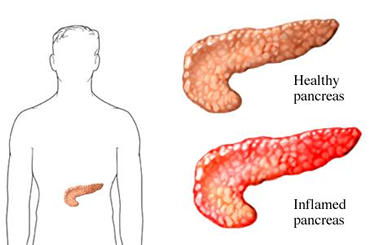
Pancreatitis can be Acute or Chronic.
Acute pancreatitis is a sudden inflammation of the pancreas that occurs over a short period of time.
Chronic pancreatitis occurs most commonly after an episode of acute pancreatitis and is the result of ongoing inflammation of the pancreas. Patients with chronic pancreatitis may suffer with severe pain and loss of pancreatic function leading to abnormalities with digestion and blood sugar.
SYMPTOMS
The symptoms of acute pancreatitis include the following:
- • Upper abdominal pain that radiates to the back, often gets worse on eating.
- • Swollen abdomen
- • Nausea
- • Vomiting
- • Fever
- • Rapid heart rate
Patients suffering from chronic pancreatitis experience constant pain that radiates to the back, nausea and vomiting, along with some of the following symptoms:
- • Diabetes - if insulin secretion is affected
- • Unintended weight loss
- • Oily stools (steatorrhea)
- • Diarrhea
- • Jaundice
CAUSES
Alcohol use is one of the most common cause identified for both acute and chronic pancreatitis. Some of the other possible causes are as follows:
- Smoking
- Gallstones or bile duct stones
- Certain medicines
- High levels of triglycerides
- Hyperparathyroidism
- Hypercalcemia
- Cancer of the pancreas
- Cystic fibrosis
- A family history of pancreatitis
- Abdominal surgery or Injury to the abdomen
DIAGNOSIS
- Medical history
- Serum Amylase and Lipase: High levels of these two enzymes strongly suggest acute pancreatitis. As the patient recovers, the digestive enzyme levels decrease to normal.
In the case of chronic pancreatitis, tests may include:
- Pancreatic function test
- Glucose tolerance test
- Ultrasound / CT Scan
- ERCP (endoscopic retrograde cholangiopancreatography)
- Esophagogastroduodenoscopy with ultrasound (EUS)
TREATMENT METHODS
In acute attack, patient needs to be hospitalized and provided with (IV) fluids for a few days along with antibiotics and pain relievers. This is done to ensure that there is no burden on the pancreas due to eating or drinking.
In the case of chronic pancreatitis, the treatment plan may include a low-fat diet, medicine to relieve pain, insulin to help with high blood sugar levels and enzyme tablets to aid digestion.
An acute attack of pancreatitis caused by gallstones may require removal of the gallbladder or endoscopic surgery of the bile duct. Laparoscopic pancreatic surgery may be advised in few cases.
People who have pancreatitis should not drink alcohol or smoke.
You may also like to learn about:
Diabetes mellitus
Abdominal pain
Pancreas divisum
Pancreatic cancer
Calculus pancreatic
Gallstones